Accessing neurologic care often presents physical, geographical and financial challenges to patients, many of whom face chronic and disabling conditions. With a nationwide scarcity of neurologists in the U.S., especially in rural areas, disparities in access to timely neurological assessment and treatment are not uncommon. Telehealth addresses access to care as well as other inequity issues.
To meet the need for prompter care and to diminish disparity for rural veterans, the U.S. Department of Veterans’ Affairs (VA) National Tele-neurology Program was funded in 2019 by the VA’s Office of Rural Health. The program is a patient-centered, flexible, cost-effective virtual hub model that uses synchronous (video) and asynchronous technologies.
In one of the first and largest studies of outpatient general teleneurology care, a research team, led by Linda S. Williams, M.D., a VA and Regenstrief Institute clinician-researcher, evaluated the innovative program which serves patients with many common conditions including headache, seizures, multiple sclerosis, recent stroke and back pain.
The researchers studied the impact the teleneurology program had on both the timeliness of access to neurological care, as well as the program’s effect on the volume of veteran neurology consultations completed outside the VA system—the only option for most Veterans prior to this new program.
“Telehealth is one way that the VA helps veterans receive care wherever they are. They don’t even have to leave their home,” said Dr. Williams. “And this is very important for some patients with conditions like epilepsy that can make driving difficult and for older patients, who may struggle to drive to a larger city that has a neurologist.
“In the VA teleneurology program, clinicians saw many common neurological problems analogous to those seen in any general neurology clinic. I think our results are likely applicable to non-VA teleneurology programs, although the VA has a very robust infrastructure for teleneurology care and for telehealth care in general, unlike many health systems,” said Dr. Williams.
The researchers compared wait times for appointments at VA sites that had implemented telecare for general neurology patients versus sites that had not yet implemented it and found shorter wait times for telehealth appointments than in-person visits. They also investigated wait times for eligible veterans to receive appointments with a community neurologist due to inability to receive an in-person appointment with a VA clinician.
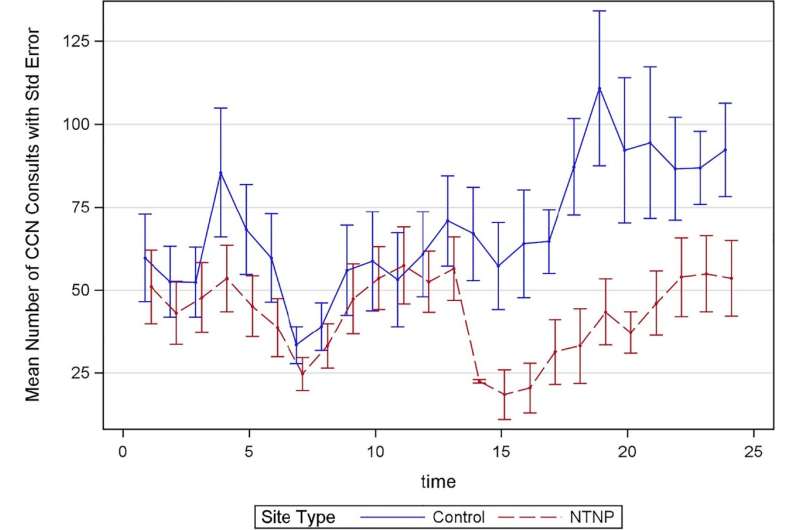
They found that sites that had implemented the teleneurology program did not see a rise in the volume of community care requests in the year after program implementation and that wait times for teleneurology were significantly less than wait times for an appointment with a community neurologist. Sites that did not implement telehealth for chronic neurologic conditions had a significant increase over time in the monthly number of community care neurology consults they placed.
Since passage by Congress of the Mission Act of 2018, veterans living more than 60 miles from a VA facility or those who must wait more than 28 days to receive care from a VA clinician are eligible to receive that care in the community. However, wait time for an appointment with a community neurologist is often quite long, especially in rural areas, where only about 3% of U.S. neurologists practice. Four out of five rural counties in the U.S. do not have at least one neurologist.
“When you implement a new program, you need to ask: Does it really make a significant difference in the outcome that you’re trying to reach,” notes Dr. Williams. With this program we were trying to improve the speed at which veterans could receive neurologic care, and we were also trying to understand, from the health care system perspective, whether implementing this new telehealth program really made a dent in the community care volume that the VA has been sending out to non-VA physicians, which has been increasing over the past few years.”
The authors conclude, “As the mismatch between the proportion of the population with neurologic conditions and the number of neurologists grows, Teleneurology outpatient care, as demonstrated by NTNP [VA National Tele-neurology Program], is one means of improving patient access to neurologic specialists.
“This care overcomes some important barriers to access, including rural residence and scarcity of local neurologists, and can be provided with high satisfaction among patients and their referring primary care providers.
“Although little randomized trial evidence exists to assess the efficacy of telehealth care for chronic conditions, and most of this literature is in patients with diabetes, our study suggests that Teleneurology care not only improves access to care but is feasible and acceptable to patients; future studies should assess the efficacy of Teleneurology care compared to in-person care for ongoing management of patients with neurologic conditions.”
The work is published in the Journal of General Internal Medicine.
More information:
Jayne Wilkinson et al, The VA National Teleneurology Program (NTNP): Implementing Teleneurology to Improve Equitable Access to Outpatient Neurology Care, Journal of General Internal Medicine (2023). DOI: 10.1007/s11606-023-08121-7
Journal information:
Journal of General Internal Medicine
Source: Read Full Article