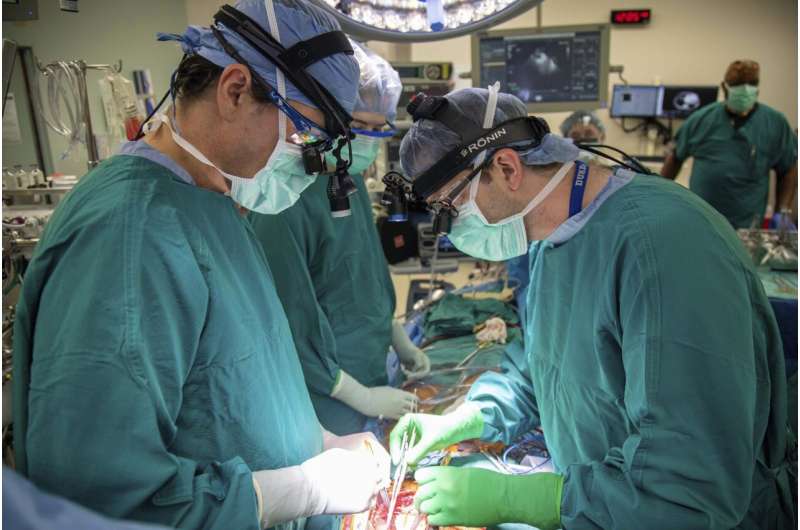
Most transplanted hearts are from donors who are brain dead, but new research shows a different approach can be just as successful and boost the number of available organs.
It’s called donation after circulatory death, a method long used to recover kidneys and other organs but not more fragile hearts. Duke Health researchers said Wednesday that using those long-shunned hearts could allow possibly thousands more patients a chance at a lifesaving transplant—expanding the number of donor hearts by 30%.
“Honestly if we could snap our fingers and just get people to use this, I think it probably would go up even more than that,” said transplant surgeon Dr. Jacob Schroder of Duke University School of Medicine, who led the research. “This really should be standard of care.”
The usual method of organ donation occurs when doctors, through careful testing, determine someone has no brain function after a catastrophic injury—meaning they’re brain-dead. The body is left on a ventilator that keeps the heart beating and organs oxygenated until they’re recovered and put on ice.
In contrast, donation after circulatory death occurs when someone has a nonsurvivable brain injury but, because all brain function hasn’t yet ceased, the family decides to withdraw life support and the heart stops. That means organs go without oxygen for a while before they can be recovered—and surgeons, worried the heart would be damaged, left it behind.
What’s changed: Now doctors can remove those hearts and put them in a machine that “reanimates” them, pumping through blood and nutrients as they’re transported—and demonstrating if they work OK before the planned transplant.
Wednesday’s study, conducted at multiple hospitals around the country, involved 180 transplant recipients, half who received DCD hearts and half given hearts from brain-dead donors that were transported on ice.
Survival six months later was about the same—94% for the recipients of cardiac-death donations and 90% for those who got the usual hearts, the researchers reported in the New England Journal of Medicine.
The findings are exciting and show “the potential to increase fairness and equity in heart transplantation, allowing more persons with heart failure to have access to this lifesaving therapy,” transplant cardiologist Dr. Nancy Sweitzer of Washington University in St. Louis, who wasn’t involved with the study, wrote in an accompanying editorial.
Last year, 4,111 heart transplants were performed in the U.S., a record number but not nearly enough to meet the need. Hundreds of thousands of people suffer from advanced heart failure but many never are offered a transplant and still others die waiting for one.
Researchers in Australia and the U.K. first began trying DCD heart transplants about seven years ago. Duke pioneered the U.S. experiments in late 2019, one of about 20 U.S. hospitals now offering this method. Last year, there were 345 such heart transplants in the U.S., and 227 so far this year, according to the United Network for Organ Sharing.
In the Duke-led study, nearly 90% of the DCD hearts recovered wound up being transplanted, signaling that it’s worthwhile for more hospitals to start using the newer method.
Sweitzer noted that many would-be donors have severe brain injuries but don’t meet the criteria for brain death, meaning a lot of potentially usable hearts never get donated. But she also cautioned that there’s still more to learn, noting that the very sickest patients on the waiting list were less likely to receive DCD hearts in the study.
Schroder said most who received DCD hearts already had implanted heart pumps that made the transplant more difficult to perform, even if they weren’t ranked as high on the waiting list.
The study was funded by TransMedics, which makes the heart storage system.
More information:
Jacob N. Schroder et al, Transplantation Outcomes with Donor Hearts after Circulatory Death, New England Journal of Medicine (2023). DOI: 10.1056/NEJMoa2212438
Nancy K. Sweitzer, Safely Increasing Heart Transplantation with Donation after Cardiac Death, New England Journal of Medicine (2023). DOI: 10.1056/NEJMe2303928
Journal information:
New England Journal of Medicine
Source: Read Full Article