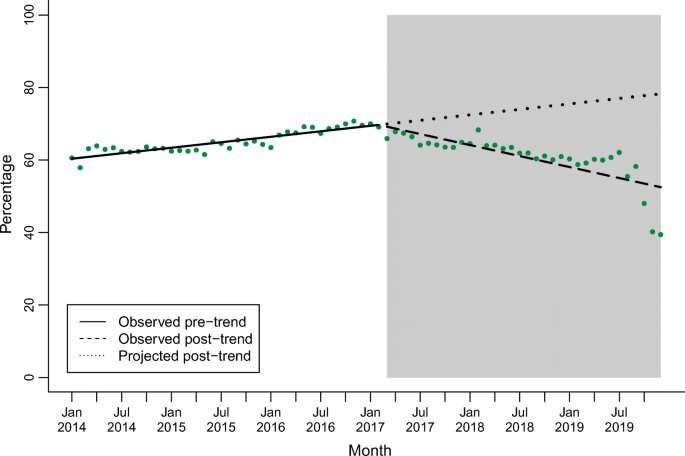
Regulation designed to reduce prescription opioid pain medications in New Jersey may not have had the intended effect: A Rutgers analysis of Medicaid records found that progression from short-term to long-term opioid use did not decline following new legislation capping initial prescriptions for acute pain to five days.
Total new prescriptions fell at a monthly rate of 0.76 per 10,000 after the rule took effect, but they had been declining at a monthly rate of 1.62 per 10,000 before policy implementation. (It’s unclear whether this change somehow stemmed from the regulations or from the fact that prescriptions had already fallen so that they couldn’t keep declining so quickly.)
The regulations did reduce the percentage of new prescriptions written for more than five days—a change that may have reduced left-over opioids available for misuse—but the same change also forced more patients who needed longer treatments to return to their doctors.
“New Jersey has been a leader among U.S. states in combatting opioid misuse,” said Stephen Crystal, director of the Rutgers Center for Health Services Research and senior author of the study. “Many of its policies have worked, and new policies designed to expand access to very effective medical treatments promise to be game-changers.”
“However,” said Crystal, who is a Board of Governors Professor in the Rutgers School of Social Work, “this policy’s apparent failure to achieve its goals illustrates the extreme difficulty of solving healthcare problems by dictating physician behavior.”
Opioid prescription rates for New Jersey Medicaid patients fell 50 percent from 2013 to 2017 after studies showing that some patients developed opioid use disorder caused the U.S. Centers for Disease Control (CDC) to tighten voluntary prescription guidelines. New Jersey’s 2017 regulation made many of the national guidelines mandatory.
The Rutgers team studied the regulation’s impact by analyzing six years of de-identified New Jersey Medicaid claims data for patients aged 18–64 who weren’t eligible for Medicare. Pharmacy claims were linked with the First Databank MedKnowledge database by National Drug Codes to identify opioid prescriptions and their duration. This data allowed them to tally the number of new prescriptions and track their duration.
Fatal overdoses from opioids and related drugs, particularly fentanyl, have rapidly become one of the nation’s leading causes of death. The CDC estimated that slightly more than 100,000 Americans died from drug overdoses for the year ended April 2021, a 29 percent increase over the past year. Opioids accounted for nearly 76,000 of those overdoses.
Still, prescription opioids serve a valuable purpose, the researchers noted. Medications such as OxyContin and Vicodin are often the most effective treatment for serious pain arising from injury and painful diseases like cancer. The apparent failure of the state regulation to suppress prescription totals further may be a good thing.
“Many people feel that we have already gone too far in reducing opioid prescriptions and denying relief to people who are in serious pain,” said Peter Treitler, a research project manager at the Rutgers Institute for Health, Health Care Policy and Aging Research and lead author of the study.
“The goal isn’t having zero opioid prescriptions; it’s having the right number going for the right duration to the right patients,” Treitler said. “That’s difficult to achieve by fiat. It’s easier to achieve by educating physicians and then giving them discretion in patient treatment, as the state is doing now in letting them prescribe medication for opioid use disorders.”
The study is published in the Journal of General Internal Medicine.
More information:
Peter Treitler et al, Association of a State Prescribing Limits Policy with Opioid Prescribing and Long-term Use: an Interrupted Time Series Analysis, Journal of General Internal Medicine (2023). DOI: 10.1007/s11606-022-07991-7
Journal information:
Journal of General Internal Medicine
Source: Read Full Article